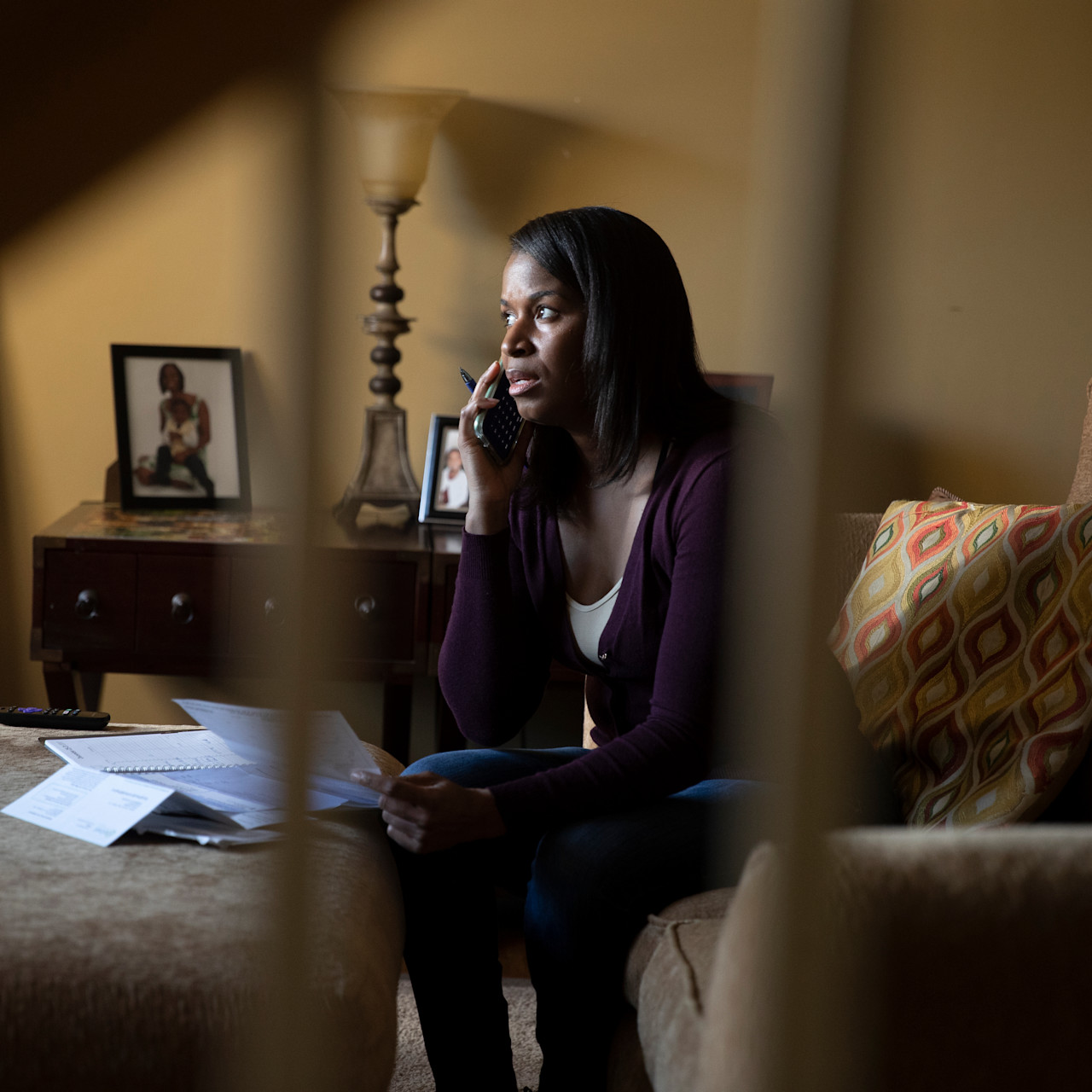Medication Access Barriers
‘There’s not really a need to go to an appointment if I can’t afford the medicine’
In this digital version of the 2021 Medication Access Report, hear from patients struggling to get the medications they need, review data on major medication access challenges and discover healthcare solutions that can make a difference.
For a deeper look into the data driving this year's report, download the full 2021 Medication Access Report.
Editor: Patient last names have been omitted to protect their privacy.
Ashley and her wife moved to Georgia in February 2020 so she could take a new job. She had recently been diagnosed with fibromyalgia and finally found a drug that helped effectively manage the major depressive disorder she also lives with.
Then COVID-19 hit.
Ashley became one of the estimated 20-million Americans who lost their jobs as well as their health insurance.COVID-19 and Medication Access, CoverMyMeds, 2020
Without health insurance, she could no longer afford her medications: Her prescription for depression alone was around $1,700 a month. While her doctor worked with her to find affordability options, each visit cost her nearly $200, even for telehealth.
“It’s been difficult to manage because there’s not really a need to go to an appointment if I can’t afford the medicine she’s going to write the prescription for,” Ashley said.

Ashley can relate to the 36 percent of patients surveyed who have given up their medications to help pay for life’s essentials.CoverMyMeds Patient Survey, 2020 Others have done the inverse: Forty-three percent said they’ve had to forgo paying for essential items and bills to afford their medications.CoverMyMeds Patient Survey, 2020 Some try to make both work: Forty-one percent said they’ve skipped or modified medication doses to stretch out their prescription.CoverMyMeds Patient Survey, 2020

To ease her fibromyalgia pain while job searching, Ashley took 800 mg of ibuprofen just to get out of bed each day. Her depression went unmanaged.

“Situational depression from (COVID-19), on top of not-having-employment depression, on top of the fibromyalgia-related depression has caused a spiral in stress and anxiety that I have never felt before,” Ashley said. “I’ve had debilitating anxiety just worrying about where our next meal is going to come from.”

While 63 percent of providers surveyed said income level affects their patients’ ability to access healthcare, only 17 percent are asking patients about their household income.CoverMyMeds Provider Survey, 2020 This layer of personal insight combined with point-of-prescribing solutions such as real-time prescription benefit (RTPB) could help prescribers open the door to pivotal patient affordability conversations.

In October 2020, after seven months without her medications, Ashley finally got a job that offered health insurance. The first things she did were schedule a surgery her wife had put off and checked the price of her medications.
“Everything is going to slowly fall back into place,” she said. “(Health insurance) takes a weight off — a weight that I can’t even describe.”

Unfortunately, insurance coverage isn’t always the key to affordability, especially since high deductible health plans encompass 46 percent of employer-based insurance plans for those under 65 and 90 percent of Affordable Care Act exchange programs.Health Insurance Coverage: Early Release of Estimates From the National Health Interview Survey, January–September 2018, National Center for Health Statistics, 2019 Patients on these plans carry the load of paying for their medical expenses most of the year — if not all of it.

Discover more data-driven insights and analysis in this year's full report — including how healthcare technology can help mitigate industry-wide affordability barriers. Download the full 2021 Medication Access Report.

Benefit Barriers
Tonia is a single mother to an active 14-year-old son. A couple years ago, he started losing patches of hair. They also noticed his fingernails starting to discolor and become brittle, “like broken glass,” Tonia said. They were so fragile they would often rip off completely and bleed from getting snagged on a shirt.
His doctor diagnosed him with pediatric psoriasis and alopecia. While she grappled with knowing her son had a chronic condition with no known cure, she was relieved to hear there was a treatment to improve his symptoms. Tonia expected to visit the pharmacy, pay for and pick up the medication and go home to start treatment with her son. Unfortunately, that would not be the case.

The pharmacist told Tonia her insurance plan required a prior authorization (PA) before she could start her son’s medication. While they went home and waited for the PA to be approved, Tonia described herself as a "nervous wreck.”
“When the medication for my son was denied, it was really disappointing, disheartening to know I wouldn't be able to go home and start the treatment process with my son,” Tonia said. “My son felt sad, defeated, frustrated, discouraged."

Tonia's story is not unique. Delays in care due to traditionally manual and multi-step benefit processes are some of the most common medication access challenges patients face. One in four patients surveyed reported a delay in receiving their medication due to PA.CoverMyMeds Patient Survey, 2020

Providers are frustrated, too. Most listed PA requests as a time-consuming part of their workday, and over half indicated they don’t have enough time to complete them.CoverMyMeds Provider Survey, 2020 Because of PA management, over one third of providers had less time for face-to-face interaction with patients — during which affordability and access conversations could occur.CoverMyMeds Provider Survey, 2020
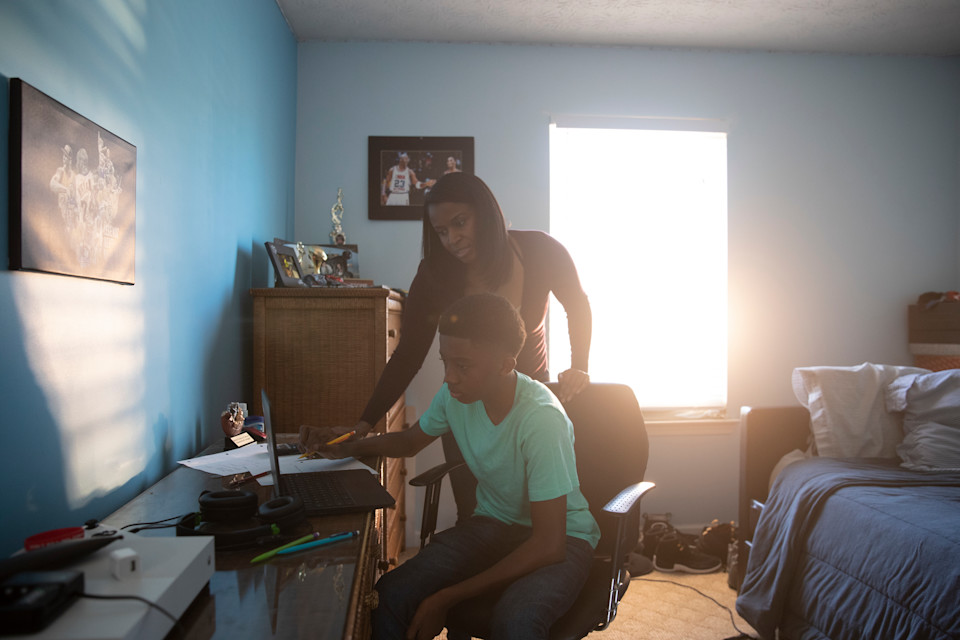
Tonia expressed what many caregivers feel when trying to manage medication access — that she’s coming up short for her son.
“It's frustrating because you think, if anything, we should all be on the same team and the goal should be to let everyone receive the medication they need, but unfortunately, for whatever reason, it's not the case,” Tonia said.

Initiating PA requests at the point of prescribing could reduce administrative burden for pharmacists and for providers later on in the process. But fewer than one in five providers do so, most waiting for the pharmacy to notify them of prior authorization requirements.CoverMyMeds Provider Survey, 2020 More than half of pharmacists surveyed reported spending at least an hour on insurance-related rejections each day, with one in five spending two or more hours daily on these tasks.CoverMyMeds Pharmacist Survey, 2020 When a PA request is submitted prospectively, at the point of prescribing, patients access their medications about 13 days sooner, on average.CoverMyMeds data on file, 2018

Integrated solutions within a provider's workflow can help speed up the PA process. Nearly all respondents are using an electronic method, and adoption of ePA increased 13 percent over last year's provider survey. CoverMyMeds Provider Survey, 2020,CoverMyMeds Provider Survey, 2019 Still, over half of providers said they are using fax to submit at least some PA requests. Nearly half are still using the phone, numbers that have remained steady over the past two years.CoverMyMeds Provider Survey, 2020,CoverMyMeds Provider Survey, 2019 Lack of interoperability between electronic systems and cost are some of the reasons these manual methods persist, decades after most industries have moved on from the fax machine.Why Your Doctor's Office Still Depends on a Fax Machine, Stanford School of Medicine, 2019 When a PA request is submitted electronically, patients can get their medication faster and are more likely to adhere to their prescribed therapy.CoverMyMeds data on file, 2019

Demographic Barriers
While costs and administrative processes can be obstacles at the pharmacy counter, other variables can also affect patients medication access. Social determinants of health — such as socioeconomic status, education, transportation options, physical living environment, race and ethnicity — have always affected healthcare, but many entered the forefront in 2020. Taking action on them may be the catalyst in shifting the healthcare industry's view from patients to people.
When surveyed, minority patients were more likely than average to be affected by finances, stretch out medication doses and make difficult decisions between their treatment and paying for essential items.CoverMyMeds Patient Survey, 2020 Three-fourths of minority patients surveyed were financially affected in some way by COVID-19 compared to just over half of white patients.CoverMyMeds Patient Survey, 2020

While many racial disparities can be linked to financial concerns, studies showed even Black Americans with high incomes and socioeconomic status are less protected from chronic medical conditions than whites of the same status.The Benefits of Higher Income in Protecting against Chronic Medical Conditions Are Smaller for African Americans than Whites, Assari, 2018 Even technology algorithms can’t always factor out the complex issue of racial bias.Dissecting Racial Bias in an Algorithm Used to Manage the Health of Populations, Obermeyer, Powers, Vogeli, Mullainathan, 2019
Race and ethnicity are among many variables to consider in healthcare technology — which is why it’s important for providers to bring the human lens to patient interactions. When deciding on the best path to medication access, providers have the opportunity to consider all variables that could impact each patient individually. Yet, one in five providers surveyed said they aren’t asking patients about social determinants of health.CoverMyMeds Provider Survey, 2020
Go deeper into this year's full report to discover more data-driven insights and analysis — including how social determinants of health impact medication access. Click here to download the full 2021 Medication Access Report.

Technology Barriers
Michael still holds the record for most cars sold in a single month at the rural Michigan dealership where he last worked seven years ago: twenty-nine, if you were curious.
“That’s pretty good at any size dealership,” he said.
He was the top salesman and finance director of the family-owned dealership in his town of 5,000 people. At 55 years old, he was putting in over 60 hours a week when he started showing symptoms of what he would soon learn was scleroderma, an autoimmune disease that affects connective tissue. Despite trying to work through the condition, Michael was forced to retire.

“I was a million-dollar seller,” he said. “With scleroderma I could not keep up; the fatigue became phenomenal. There was no way I could work those hours. I tried.”
Michael had trouble finding a good rheumatologist near his rural town. The provider he finally found was located two hours away in Ann Arbor. While telehealth was an option, Michael preferred face-to-face appointments, especially since scleroderma affects the skin, making examinations difficult over video calls. Internet connectivity issues and the impersonal feeling of virtual interactions added to his dislike for telehealth.

An online healthcare aspect Michael does appreciate are virtual patient support groups. While finding a scleroderma, or even a general patient advocacy group, would be a tall order in his area, Michael has been able to connect with other patients around the globe through social media. They discuss symptom management, medications and other hurdles to chronic conditions such as insurance authorizations, affordability and provider access. Michael leads many of the groups and even leads online webinars to help patients find the right path to disease management.
“There are ways to navigate the system, but most people, when they’re fighting a disease that they can’t even get out of bed with some days and don’t have the stamina, they lose the will to fight, they give up,” Michael said. “And I don’t want anyone to give up. I want to help people.”

Fewer than one in three providers surveyed said they ask patients about their access to technology and mass media.CoverMyMeds Provider Survey, 2020 But nearly half said it’s a factor that impacts their patients’ ability to access healthcare; the same number indicated patients’ skill level with technology impacts healthcare access.CoverMyMeds Provider Survey, 2020

A social determinants of health screening could identify patient technology disparities — especially important as telehealth use has ramped up. This information, integrated into EHR and patient-accessible portal data, could help physicians make better prescribing decisions. This easy-to-access prescription decision technology, inclusive of RTPB and ePA, can continue to support providers for their patients who choose telehealth to expedite appointments and improve medication adherence.

Healthcare Consumerism
‘I think there’s a lot to be said for how comfortable you feel when you’re at home’
In this digital version of the 2021 Medication Access Report, hear from patients struggling to get the medications they need, review data on major medication access challenges and discover healthcare solutions that can make a difference.
For a deeper look into the data driving this year's report, download the full 2021 Medication Access Report.
Editor: Patient last names have been omitted to protect their privacy.
Kathy has always been a proactive consumer and patient. Before grocery delivery and instant pickup were dreamt of, she contacted the manager of her local market to have her groceries brought to her car to avoid illness and the hassle of bringing two small daughters into the store. When she was diagnosed with multiple sclerosis (MS), her prudent consumer savviness became even more important. Fast-forward to the COVID-19 pandemic, and she’s done everything in her power to stay healthy while being immunocompromised.
“I’m scared to go any place,” she said.

When her neurologist ordered routine bloodwork, she asked if they could use results of a full panel draw she’d had during a recent emergency room visit.
“That’s the way I’m thinking now,” she said. “I don’t want a stick unless I need it and (I consider) cost, and I don’t want to go somewhere and get exposed either.”
For the same reason, Kathy said she’s grateful for the increase in telehealth appointments over the past year. Even after the initial spike in spring 2020, telehealth use remained exponentially higher than ever — over 2,000 percent higher than baseline levels through the end of 2020 — indicating a more permanent option for provider access.Monitoring the Impact of COVID-19 on the Pharmaceutical Market, IQVIA, 2020

Over 54 percent of providers surveyed said telehealth was an available option for all of their patients.CoverMyMeds Provider Survey, 2020 Of the 70 percent of patients surveyed who had participated in a telehealth appointment, over half said they did so for the convenience.CoverMyMeds Patient Survey, 2020 More than one in five said they participated because it gave them more control over their healthcare.CoverMyMeds Patient Survey, 2020
Go deeper into this year's full report to discover more data-driven insights and analysis — including how patients are becoming part of the care team. Download the full 2021 Medication Access Report.

Kathy pointed out that, for some, taking an appointment from home can open up an entirely new dialogue with providers.
“I think there’s a lot to be said for how comfortable you feel when you’re at home,” she said. “I felt like I remembered more that I wanted to talk to the doctor about because I wasn’t so nervous.”
During a telehealth appointment, healthcare solutions that allow pull-through functionality to patient-facing portals can give patients easy reference to their health information, such as vital sign history, diagnostic details and medication information.
And for providers, a glimpse into a patient’s home life can better inform prescribing and healthcare decisions.

“They can be scanning to know a little bit more about you and your lifestyle and that might lead to more conversation,” Kathy said. “I would hope in the back of their mind there’s some sort of integrative quality to recognize, ‘Oh, you have a dog! Good, do you take that dog for a walk?’
“I just think it gives a lot more opportunity to open up the dialogue and be a little more holistic, and for the patient, (telehealth) makes it much easier and much calmer.”

The results of her appointments — including labs, tests and prescriptions — can be a little more hectic to coordinate, especially when ferrying information among multiple care team members such as specialists, primary care providers and specialty pharmacists. Unfortunately, healthcare lags an estimated 10 years behind other industries when it comes to using technology to improve consumer engagement.Independent Study Commissioned by Virtusa Finds 85 Percent of Businesses Plan to Invest in Digital Transformation in 2018, Businesswire, 2018 Lack of interoperability between electronic systems and cost are some of the reasons these manual methods persist, decades after most industries have moved on from the fax machine.Why Your Doctor's Office Still Depends on a Fax Machine, Stanford School of Medicine, 2019
“When (electronic medical records) first came out, I was so excited because I thought, ‘This is going to be seamless,’ which is the way it should be,” Kathy said. “But they all are in their different data bubbles.”
Kathy appreciates having her health information in a patient portal so she can monitor her numbers and conduct her own research if she has questions. This processing time can be important, especially since patients forget 40 to 80 percent of the information from their appointments — and of what they do remember, half is incorrect.Patients' memory for medical information, Kessels, 2003

Patients are often responsible for sharing their drug history, lab data and condition information among several providers.Confronting The Growing Burden Of Chronic Disease: Can The U.S. Health Care Workforce Do The Job?, HealthAffairs, 2009 Provider tools can help digitally surface drug information literature from pharmaceutical companies so patients can more easily expand their health literacy and advocate for their condition management, helping improve potential outcomes.

Affordability can also make a difference when it comes to medication adherence. Apps that promote patient choice in pharmacy and medication can be crucial. While patients are willing to prescription price-shop, they don’t often know where to start or what’s available. Sixty-two percent said they actively asked their provider about medication price and affordability options.CoverMyMeds Patient Survey, 2020 When patients were faced with a prescription that cost more than they expected, 43 percent used price shopping tools to find a better price — up from 28 percent last year.CoverMyMeds Patient Survey, 2020,CoverMyMeds Patient Survey, 2019
“There’s a lot of coordination that goes on that I don’t feel like the patient should have to do,” Kathy said. “Not everybody is as lucky as I am. The kind of stress that goes into finding (financial) assistance and coordinating … I don’t think you can downplay that effect on someone’s health.”

Patient Engagement
‘I was struggling and feeling really bad, and he could tell in my mannerisms’
In this digital version of the 2021 Medication Access Report, hear from patients struggling to get the medications they need, review data on major medication access challenges and discover healthcare solutions that can make a difference.
For a deeper look into the data driving this year's report, download the full 2021 Medication Access Report.
Editor: Patient last names have been omitted to protect their privacy.
Dennis and his daughter, Annie, then 21, stood together at the bottom of a steep incline in the French Alps in August 2019. Annie turned to her dad with a challenge in her eye, as she always did on their travels when they came to a staircase or ascent.
“Race ya,” she said.
The pair took off running, and for the first time ever, Dennis reached the top before her. When he turned around, he found disbelief in Annie’s face. It wasn’t just that her dad, nearing 70, had beat her in a race. A couple years earlier, his lungs were only operating at 66-percent capacity due to severe asthma. The fact that he made it up the hill at all was astounding. He credits finding the right prescription medication and his enthusiastic, informed specialist for his nearly fully restored lung function.

“In most (doctor’s) appointments, we all hope or wish there was something new,” Dennis said, recalling his visit to the specialist earlier that year. “But this time there was a breakthrough, and (my doctor) was excited about it because she knew what it would mean to those of us afflicted.”
Though the breakthrough medication made a dramatic difference in his lung health, the price tag took his breath away: a $700 insurance copay each month. He talked with his doctor about affordability options. Luckily, she had some free samples to offer him that lifted the financial burden for a few months.

Patient-provider trust can make or break medication access barriers. Over a third of patients said they avoided asking their provider about medication affordability, while more than 60 percent of providers said they may wait for the patient to bring up financial concerns before discussing medication price and affordability.CoverMyMeds Patient Survey, 2020,CoverMyMeds Provider Survey, 2020 This chess match benefits no one.
After the COVID-19 economy created financial strain and the free samples ran out, Dennis had to make a hard choice.
“I had stopped taking this wonderful drug that had improved my lung health because I could no longer pay for it,” he said.
This isn’t uncommon: Two-thirds of patients surveyed went to pick up a prescription only to find it cost more than expected.CoverMyMeds Patient Survey, 2020 As a result, over a third of those patients abandoned their medications.CoverMyMeds Patient Survey, 2020 On top of financial concerns and going without his medication, Dennis also endured significant changes in his personal life as a long-term relationship came to an end and he was forced to relocate.

“COVID is almost a sideshow for me,” Dennis said. “Imagine ending a relationship and moving from the home you've lived in for years amid a pandemic.”
His primary care provider reached out to patients after COVID-19 office closures to set up “check-in” telehealth appointments, especially for patients experiencing hardships due to the recent pandemic. It was during this appointment that his provider noticed — even through a computer screen — something was different about Dennis.

“I was struggling and feeling really bad, and he could tell in my mannerisms,” he said. “It was an amazing moment.”
One positive aspect of telehealth some providers noted was a better understanding of their patients as people.Have EHRs Been a Burden or an Asset During the Coronavirus?, EHR Intelligence, 2020 Seeing patients in their own homes can bring providers closer to the things patients care about most — which can help providers make better care and prescribing decisions. By understanding the many pressures and facets of patients’ lives, providers can better understand the best care plan for patients and, further, collaborate on the best way for them to access medications.
Go deeper into this year's full report to discover more data-driven insights and analysis — including how technology solutions can support the care team. Download the full 2021 Medication Access Report.
The provider prescribed a medication to help treat depression that Dennis said made a dramatic difference during a challenging year.
Eighty-six percent of providers surveyed reported having a positive experience using telehealth, with one-third of providers noting decreased patient no-show rates.CoverMyMeds Provider Survey, 2020 Unfortunately, nearly 40 percent noted an increase in administrative burden, as telehealth appointments often involve a single provider handling all aspects of a patient visit.CoverMyMeds Provider Survey, 2020,Pandemic-era burnout: How physicians manage crushing workloads and IT demands, Healthcare IT News, 2020

Integrated technology that provides visibility into medication payment and alternative options can aid the improvement of telehealth by aggregating more tools in one location. When supported by point-of-prescribing solutions that offer affordability options, medication information and ePA, providers can fully address patient concerns, whether through a screen or in-person.

Patient relationships with their pharmacists could also benefit from improved conversations and tools to buoy them. More than half of patients surveyed said they asked their pharmacist or provider about cheaper alternatives when their prescriptions cost too much.CoverMyMeds Patient Survey, 2020 And providers and pharmacists agreed the task of helping patients find medication affordability options most often fell on pharmacists.CoverMyMeds Provider Survey, 2020,CoverMyMeds Pharmacist Survey, 2020

Patients like Kathy (who was featured in the healthcare consumerism section of the 2021 Medication Access Report) are recognizing pharmacists’ evolving role as providers more often.
“I think pharmacists are one of the most important parts of what I call my healthcare advisory board,” Kathy said. “I have no hesitancy to pick up a phone and call there. They’re easy to get through to and the doctors are not.”
Seventy-two percent of patients regularly asked their pharmacist questions about medications.CoverMyMeds Patient Survey, 2020 Pharmacists said the questions they answer are most often about medication price, drug information, alternative affordability options and PA status.CoverMyMeds Pharmacist Survey, 2020 Pharmacists also most want to see these pieces in their ideal tool, with PA status topping the list.CoverMyMeds Pharmacist Survey, 2020

Pharmacists need tools to effectively field patient questions and problem-solve when affordability issues come up. Staying in-workflow is critically important: 82 percent of pharmacists said it’s important or very important to integrate their ideal tool into their current pharmacy dispensing system.CoverMyMeds Pharmacist Survey, 2020 Pharmacists using an integrated solution including real-time PA status updates saw a 14 percent increase in paid claims, on average.CoverMyMeds data on file, 2019

Patient Support Services
‘I don’t know how people can afford to be sick and still live their lives.’
In this digital version of the 2021 Medication Access Report, hear from patients struggling to get the medications they need, review data on major medication access challenges and discover healthcare solutions that can make a difference.
For a deeper look into the data driving this year's report, download the full 2021 Medication Access Report.
Editor: Patient last names have been omitted to protect their privacy.
A chronic condition diagnosis is a life interrupted. It can stymie daily routines, curtail hobbies and even lead to unemployment when lack of energy and symptoms interfere with job tasks.
As the manager of a 401K processing group, an avid cyclist and traveler, Patricia didn’t know the word “stop.” Then she woke up one morning unable to see. After a series of trips to the emergency room, diagnostic tests and several specialist visits, she was finally diagnosed with MS.
But she had things to do.
“I had a bicycle ride (coming up), and I just wanted to know if I would be OK to ride my bike to Montreal,” Patricia said. “They said, ‘We need you to take this seriously.’”

Her doctors recommended an MS drug administered through an infusion every six months. While grateful for an option to help manage her symptoms — she had lost 25 percent of her vision in both eyes and could no longer drive — Patricia was hesitant.
“I struggled to say, ‘Schedule me for the infusion,’” she said. “I spent most of my savings going from doctor to doctor. I’m not sure what answer I was looking for. I was looking for something less invasive.”
Patricia finally decided to try the infusion when she came up for a promotion at work. She didn’t want her MS symptoms to interfere with her new responsibilities. Then she heard the price: a $6,500 copay for each infusion, with what she was told was very good insurance through her employer.
Of patients with employer-sponsored insurance at large firms (200+ workers), 45 percent have a plan with at least one specialty drug cost-sharing tier.2020 Employer Health Benefits Survey, Kaiser Family Foundation, 2020 Most of the time, the higher a drug is in a tiered system, the more of the cost patients are responsible for.Marketplace Pulse: Cost-Sharing for Drugs Rises Sharply at Higher Tiers, Robert Wood Johnson Foundation, 2019 Among patients at large firms in a plan with at least one separate tier for specialty drugs, 53 percent have coinsurance, with an average rate of 26 percent.2020 Employer Health Benefits Survey, Kaiser Family Foundation, 2020
Go deeper into this year's full report to discover more data-driven insights and analysis — including more about the future of accessing specialty therapies. Download the full 2021 Medication Access Report.
Those in high deductible health plans are more likely to either have the same cost-sharing regardless of drug type or to meet the plan deductible before drug costs are covered.2020 Employer Health Benefits Survey, Kaiser Family Foundation, 2020

Per capita specialty medicine spending has nearly doubled since 2009, representing $517 out of the $1,044 total per person medicine costs in 2018.Medicine Use and Spending in the U.S.: A Review of 2018 and Outlook to 2023, IQVIA, 2019

“I was still trying to plan my vacations, and it became vacations or MS treatment,” she said. “I don’t know how people can afford to be sick and still live their lives. So, I opted out. I canceled (the infusion).”
Patients are more likely to abandon specialty therapies than any other drugs during the deductible period of their insurance, possibly leading to worsening conditions and future hospitalization.Medicine Use and Spending in the U.S.: A Review of 2018 and Outlook to 2023, IQVIA, 2019
“I take it one day at a time and hope … I’m not going to find out when it’s too late that I really should have been on medication.”

Specialty Therapy Access Barriers
While the high cost of specialty medications can feel like a staggering barrier, simply accessing therapy can prove even more difficult. Kathy said the stress of juggling multiple provider expectations and test results to manage her MS can trigger cognitive fog or “cog fog,” a momentary loss in mental clarity.
“I have had full-on ‘cog fog’ flares after having to deal with this stuff,” Kathy said. “It’s too much to ask a patient to have to do, and it has affected my health, no question.”


Patients have to spend the “good” days of their chronic conditions managing those conditions. They spend the other days just getting by.
Eighty-two percent of those prescribed specialty therapy reported spending an hour on the phone coordinating care to begin specialty therapies.CoverMyMeds Patient Survey, 2019 Over a third spent at least three hours.CoverMyMeds Patient Survey, 2019 Specialty hub programs designed to navigate the process of starting and maintaining complex therapies can help alleviate this time burden. Providers can direct patients to specialty hub programs designed to provide centralized patient services for financial assistance, benefit coordination, pre-therapy support and managing adherence programs. Ideal hub programs allow providers to enroll patients electronically for a seamless transition to therapy.
Patients can then electronically navigate affordability, benefit verification, pharmacy access and medication mode of delivery. In some cases, such inclusive patient support services have contributed to a 34 percent reduction in time to therapy.CoverMyMeds data on file, 2020

COVID-19 disrupted specialty medication distribution and administration, but the shifts to keep patients out of facilities may have opened doors to more accessible therapies. Data shows that many patients who receive provider-administered drugs in hospitals or facilities shifted to self-administered oral, patient-injectable or home infusion drugs.Monitoring the Impact of COVID-19 on the Pharmaceutical Market, IQVIA, 2020 Many payers relaxed restrictions on home infusions to allow specialty patients improved access to their medications.RIN 0938-AU31 Medicare and Medicaid Programs; Policy and Regulatory Revisions in Response to the COVID-19 Public Health Emergency, Department of Health and Human Services, 2020

While the pandemic revealed many shortcomings and risk areas for those living with chronic conditions, it also revealed the resiliency of the industry and, more strikingly, of patients.
“When COVID hit and people were social distancing, I had it a little easier than people who were not struggling with an autoimmune disease,” Patricia said, referencing her caution while living with MS. “People had to figure out what life would look like when your world has to slow down but the rest of life is still going.”
As we move toward a COVID-19 vaccine and learning how to navigate a world beyond the pandemic, patients with chronic conditions will still need ways to manage their care.
“MS turned my world upside down,” Patricia said. “COVID did not turn my world upside down.”
Explore Other Sections
Press inquiries:
media@covermymeds.com
Advisory Board
The Medication Access Report is developed in consultation with an advisory board of healthcare experts representing major organizations across the industry — each with unique perspectives, interests and opinions.